One of the central aims of the new Patient Safety Incident Response Framework (PSIRF) is to ensure we have compassionate engagement with patients and families, doing this well has been something that organisations have struggled with for years.
This was bought home to me a couple of years ago when we were working with a care home providing support for people with learning disabilities, we were conducting a culture survey with the staff team when one of the residents said to the Manager ‘why aren’t you asking us about this?’
This comment really struck me and the whole team, of course we should be asking residents about their perceptions of safety, it is their home after all!
So, as a team we looked at what we could utilise and decided the PRASE tools could be perhaps be used for this purpose?
What is PRASE?
PRASE is an evidence-based and validated data collection and reporting tool based on the Yorkshire Contributory Factors Framework (https://improvementacademy.org/resource/yorkshire-contributory-factors-framework/ ). The tool was developed by the Yorkshire Quality and Safety Research Group.
By asking about contributory factors PRASE aims to identify things that could lead to harm before the harm occurs so staff and patients/service users can take action.
The tool asks about: Communication & Teamwork; The Environment; Access to Resources; Organisation & Care Planning; Information Flow; Staff Roles and Responsibilities; Delays to Care; Staff Training; and Dignity and Respect.
Feedback is collected independently of the staff caring for the patient. When feedback has been collected from a minimum of 20 patients/service users, a safety report is generated. This report is discussed by all the people caring for patients and service users to identify areas to celebrate and areas that need improvement. All this reduces the likelihood of safety events happening.
For an overview of PRASE please watch Professor Rebecca Lawton’s video below:
It has been used on over 30 wards, several Emergency Departments, and a care home group. We have learnt that:
- Patients and service users certainly can tell us about safety and also provide information about when safety failures are more likely to occur.
- The information collected from patients and service users differs from other forms of safety intelligence already collected, e.g. case note review, staff incident reporting and patient complaints, and therefore does not duplicate effort.
- Staff are extremely positive about the use of PRASE feedback for making ward improvements and that the information provided is suitable to support effective action planning.
Co-designing and adapting the PRASE tools to suit different contexts
Whilst there is plenty of evidence that PRASE tools can be used to collect valid patient safety insights that staff recognise to be useful, these tools were originally designed and tested in acute hospital ward settings. In order to adapt to different care contexts and ensure meaningful data is collected, we have co-designed some alternative versions for use in care homes and Emergency Departments.
For our work in care homes we took the tools and our learning about how to apply and focussed on some of the core questions. We spent time co-designing with residents both the question wording, fitting them to the care home context and designing what the feedback report should look like for maximin impact.

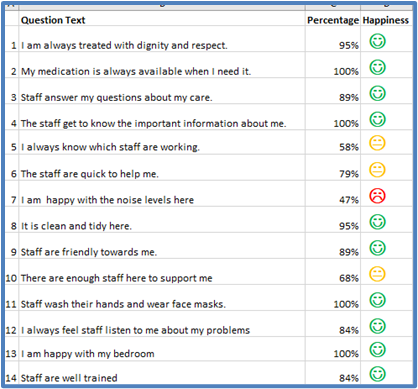
In the care homes we looked at what staff had told us in their culture survey and discussed this with residents along with results from their PRASE surveys.
Insights were captured in the form of posters visible to all, some ideas for improvements were made for example around residents not knowing who was going to be supporting them each day and how to reduce noise levels in the home.
For an ED context, because of the busy environment, we were interested in using a shorter version. We worked with a pilot ED to choose the 10 most pertinent questions for them from our bank of PRASE survey questions. We have also experimented on the best time to use these with patients – during their visit, or via a follow-up call (with permission) when they get home; both approaches have pros and cons.
We therefore now not only have a range of data collation tools available, but a range of resources and expertise to support their effective use, as well as coaching support for making improvements involving staff and patients/service users.
To return to our original lightbulb moment; of course, we should be asking patients, service users and care home residents for their insights around safety. Their perceptions are unique and can really help care teams make improvements.
If you would like support using these resources contact the team on academy@yhia.nhs.uk